Language: Spanish
References: 21
Page: 20-26
PDF size: 225.97 Kb.
ABSTRACT
Objective: To define which would be the mechanical power (using a
mathematical model that can apply to possible causes for lung injury) used by a
ventilator, in patients undergoing invasive mechanical ventilation in spontaneous
PAV (proportional assist ventilation).
Material and methods: The mechanical and distention powers are calculated using the equations:
| 1. Poder mecánico rs = |
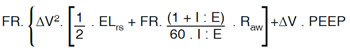
|
2. Mechanical power
rs = (0.098) . (FR . ΔV) . (P
peak - ˝ . ΔP)
3. PD = (0.098) . (P
PL- PEEP) . Vt . RF
Sixty patients were selected, half of them with invasive mechanical ventilation PAV in spontaneous mode, estimating the plateau pressure (P
pl) though tidal volume value (Vt), distensibility (C
rs), and the positive pressure at the end of a normal exhalation (PEEPt) given by the mechanical ventilator.
Results: Data from 60 patients undergoing invasive mechanical ventilation was included, 30 of them through spontaneous modality: proportional assist ventilation (PAV), from which 100% had a successful ventilator tube removal; 30 patients were paired as controls with controlled modalities, with age 65 years (SD ± 15), 63% were men, with the general parameters: mean respiratory frequency (RF) of 18 (SD ± 5.5) min-1, mean Vt of 0.46 (SD ± 0.1) Lts, mean C
rc of 55 (SD ± 22) mL/cm H
2O, PEEPt of 7.6 (SD ± 3.3) cm H
2O, peak pressure (Ppico) 20.4 (SD ± 6.9) cm H
2O, Ppl of 17.05 (SD ± 5.8) cm H
2O. When comparing the mechanical power, all the results were inferior in patients with spontaneous modality versus patients undergoing controlled modality ventilation, determining the following values: 6.98 (SD ± 1.69) versus 18.49 (SD ± 8.20) J/min (p ‹ 0.001), 7.17 (SD ± 1.67) versus 20.92 (SD ± 9.05) J/min (p ‹ 0.001) and of 4.6 (SD ± 1.64) versus 12.33 (SD ± 7.04) J/min (p ‹ 0.001), in the equations 1, 2, and 3 respectively, with an average value for the patients undergoing spontaneous modality of 6.25 (SD ± 1.66) J/min.
Conclusions: The probability of determining a mean value for the mechanical power used in patients undergoing invasive mechanical ventilation on a PAV mode may allow to obtain a standard parameter to follow under the context of its estimated equivalence in physiological conditions, mainly for patients in whom lung protective measures are desired in order to obtain a positive progress and the eventual removal of the invasive ventilation.
REFERENCES
Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, et al. Acute respiratory distress syndrome: the Berlin defi nition. JAMA. 2012;307(23):2526-2533.
Amato MB, Barbas CS, Medeiros DM, Magaldi RB, Schettino GP, Lorenzi-Filho G, et al. Effect of a protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med. 1998;338(6):347-354.
Villar J, Kacmarek RM, Pérez-Méndez L, Aguirre-Jaime A. A high positive end-expiratory pressure, low tidal volume ventilatory strategy improves outcome in persistent acute respiratory distress syndrome: A randomized controlled trial. Crit Care Med. 2006;34(5):1-8.
The Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342:1301-1308.
Ferguson ND, Frutos-Vivar F, Esteban A, Anzueto A, Alia I, Bower G, et al. Airway pressure, tidal volume, and mortality in patients with acute respiratory distress syndrome. Crit Care Med. 2005;33(1):21-30.
Jardin F, Vieillard-Baron A. Is there a safe plateau pressure in ARDS? The right heart only knows. Intensive Care Med. 2007;33(3):444-447.
Amato MB, Meade MO, Slutsky AS, Brochard L, Costa EL, Schoenfeld DA, et al. Driving pressure and survival in the acute respiratory distress syndrome. N Engl J Med. 2015;372:747-755.
Guérin C, Papazian L, Reignier J, Ayzac L, Loundou A, Forel JM, et al. Effect of driving pressure on mortality in ARDS patients during lung protective mechanical ventilation in two randomized controlled trials. Critical Care. 2016;20:384.
Li-Chung Chiu, Han-Chung Hu, Chen-Yiu Hung, Chih-Hao Chang, Feng-Chun Tsai, Cheng-Ta Yang, et al. Dynamic driving pressure associated mortality in acute respiratory distress syndrome with extracorporeal membrane oxygenation. Ann Intensive Care. 2017;7:12.
Gattinoni L, Carlesso E, Caironi P. Stress and strain within the lung. Curr Opin Crit Care. 2012;18(1):42-47.
Laffey JG, Bellani G, Pham T, Fan E, Madotto F, Bajwa EK, et al. Potentially modifi able factors contributing to outcome from acute respiratory distress syndrome: the LUNG SAFE study. Intensive Care Med. 2016;42:1865-1876.
Chiumello D, Carlesso E, Cadringher P, Caironi P, Valenza F, Polli F, et al. Lung stress and strain during mechanical ventilation for acute respiratory distress syndrome. Am J Respir Crit Care Med. 2008;178:346-355.
Protti A, Maraffi T, Milesi M, Votta E, Santini A, Pugni P, et al. Role of strain rate in the pathogenesis of ventilator-induced lung edema. Crit Care Med. 2016;44(9):e838-e845.
Cressoni M, Gotti M, Chiurazzi C, Massari D, Algieri I, Amini M, et al. Mechanical power and development of ventilator-induced lung injury. Anesthesiology. 2016;124(5):1100-1108.
Gattinoni L, Tonetti T, Cressoni M, Cadringher P, Herrmann P, Moerer O, et al. Ventilator-related causes of lung injury: the mechanical power. Intensive Care Med. 2016;42(10):1567-1575.
Marini JJ, Jaber S. Dynamic predictors of VILI risk: beyond the driving pressure. Intensive Care Med. 2016;42(10):1597-1600.
Guérin C, Reignier J, Richard J, Beuret P, Gacouin A, Boulain T, et al. Prone positioning in severe acute respiratory distress syndrome. N Engl J Med. 2013;368:2159-2168.
Fujita Y, Fujino Y, Uchiyama A, Mashimo T, Nishimura M. High peak inspiratory fl ow can aggravate ventilator-induced lung injury in rabbits. Med Sci Monit. 2007;13(4):BR95-100.
Mead J, Takishima T, Leith D. Stress distribution in lungs: a model of pulmonary elasticity. J Appl Physiol. 1970;28(5):596-608.
Cressoni M, Chiurazzi C, Gotti M, Amini M, Brioni M, Algieri I, et al. Lung inhomogeneities and time course of ventilator-induced mechanical injuries. Anesthesiology. 2015;123(3):618-627.
Suarez-Sipmann. Ventilación asistida proporcional. Med Intensiva. 2014;38(4):249-260.
